
By Khadija Diallo, Project Assistant, Project on Family Homelessness
Kianna is 17 years old. She suspects that she has depression. She only recently started experiencing symptoms of her mental illness, so she’s having a hard time adjusting. To complicate her situation, she’s homeless along with the rest of her family. Her parents lost their jobs in January and could no longer afford rent. They ended up having to move from shelter to shelter.
Her family sees her struggling more with their situation than they are and they feel helpless. Her mom cries herself to sleep every night wondering what broke her daughter down to the point that she’s contemplating suicide. Kianna needs some outside help. Perhaps a counselor and a detailed medication plan could help her get through her depression. But she doesn’t know where to turn to for help. Her family wants to help her get through her challenges, but they don’t know how to be supportive of her condition.
I created this scenario based on my observations and my research because I want people to know that mental illness doesn’t only affect the person dealing with it, but every member of that person’s family. Its impact is significant; no parent wants to see their child struggle through a mental illness. No older sibling wants to see their sister or brother battling an illness and feel helpless.
Luckily, that’s where organizations like Sound Mental Health (SMH) and the National Alliance on Mental Illness (NAMI) come in.
My query: Mental illness and family homelessness
For a while, I have been interested in learning about the impact of mental illness in homeless families.
My family’s been affected by mental illness, and I was wondering about the added challenge of dealing with a mental illness while being homeless. At first, I thought finding more data on this would be easy, but getting the information I truly wanted, such as the effects on the family members of the homeless person dealing with a mental illness, was much harder than I had anticipated. What about homelessness’ impact on the mental wellbeing of children?
(Note: If you’re interested in learning more about the relationship between homelessness and the long-term impacts on health and mental health, read our former project coordinator Perry Firth’s post on Adverse Childhood Experiences.)
According to the National Coalition for the Homeless, “for homeless families, mental illness was mentioned by 12 percent of cities as one of the top 3 causes of homelessness,” in a survey by the U.S. Conference of Mayors.

This year’s Count Us In point-in-time count of homelessness in King County shed a little bit of light on the information that I was looking for: How many homeless people are dealing with a mental illness?
According to the just-released figures, 45 percent of the 1,158 homeless people surveyed by All Home reported a psychiatric or emotional problem. That’s even higher than the one-third of the homeless population that we often hear about.
I also learned about the impact of homelessness on the physical and mental health of children, as well as their academic success, in this Firesteel series by our former project coordinator Perry Firth.
To get further answers to my questions, I interviewed Lauren Simonds, executive director of the National Alliance on Mental Illness (NAMI)-Washington; Stephen McLean, PR and marketing director at Sound Mental Health (SMH); and Annamaria Gueco, who oversees the supportive housing program at SMH. Here is what I learned.
Sound Mental Health — A pathway to recovery
On average, Sound Mental Health serves 20,000 men, women and children annually throughout the King County area. There are 13 locations, mostly serving clients on an outpatient basis. They also serve families through their Child and Family Services program, which specializes in both individual and family therapy.

Mental Illness and Homelessness: What is the link?
As for the intersection of mental illness and homelessness, McLean believes there is a strong link between the two.
“Often, untreated mental illness can eventually lead to the destruction of relationships, loss of jobs, and of course, the loss of homes and places to live,” he said. “For some people, like youth, traumatic events (sexual and other) experienced during times living on the street can increase risk for substance [abuse] and other issues.”
McLean also said that there’s a difference between treating stably housed clients and clients who are homeless, and that as you would guess, the lack of a stable home can pose challenges for clients experiencing homelessness.
“I don’t think there’s an argument that when we address a client’s basic needs – shelter, food, security, they are more receptive to accessing (or considering accessing), behavioral health and substance-use service,” he explained. “Because we use an assertive model, meaning often we go to where our clients are, having a stable house also means we have a way to contact and engage clients.
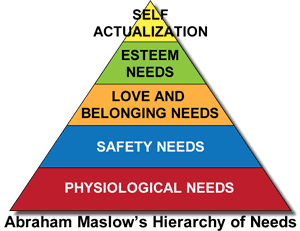
“Homeless clients are difficult to reach and engage, largely due to no physical address. So when people’s basic needs — think Maslow – are being met, they are both receptive to support and they are easier to reach and sustain support.”
Talking to Steve led me to want to know more about how SMH assists members of families who are homeless. How do families who are homeless and uncertain of where they may be sleeping make and keep appointments, for example?
Annamaria Gueco (who, as mentioned earlier, oversees the supportive housing program at SMH), says most of the homeless families they work with are in shelters. “We’re working with them, meeting with them in the community, getting them into housing. We deal with the client. It’s a really integral part of the program.”
As for a typical scenario of a client who is from a family experiencing homelessness, Gueco believes there are no uniform characteristics:
“Each family is unique and individual. What we’re seeing is many of them, head of households, experienced homelessness in their childhood, vocalized being homeless or having experienced a traumatic childhood whether that be abuse, sexual trauma and are currently experiencing trauma. Those are common themes.”
NAMI: Another resource for homeless families dealing with mental illness

To make a difference, we need not only service providers like Sound Mental Health, but advocacy organizations trying to change policy. I got into contact with Lauren Simonds of NAMI Washington to learn more about how a grassroots organization can help change the prospects of families struggling with mental illness.
NAMI is one of the nation’s largest grassroots mental health organization dedicated to, as they put it, “building better lives for the millions of Americans affected by mental illness.” The organization operates at the national, state and local level. NAMI offers peer-educated classes to help cope with mental illness and to help friends and family members of individuals affected by mental illness.

NAMI WA had an exhibitor table at the Washington Low Income Housing Alliance Conference on Ending Homelessness earlier this month. I wondered why they were there. Simonds explained that because an estimated one-third of the homeless population have a mental illness, it’s important for her organization to widen its services to a larger network of people, to help families cope with mental illness.
What I Learned
From my research, I wasn’t able to learn as much as I wanted to about the relationship between homelessness and mental illness. Perhaps I wasn’t asking the right questions, or I just didn’t know how to best ask the questions to get to the heart of the answers. It’s really difficult to research and talk about mental illness and homelessness, maybe because it’s such a sensitive topic. Despite the prevalence of mental illness in our society, it still has stigma attached to it.
I wish there weren’t a stigma surrounding mental illness. I understand that people want to keep parts of their lives private, but a mental illness should be vocalized in order to be properly treated. For homeless families, it’s understandable that they would be more at risk for illnesses like depression, anxiety and PTSD. But there shouldn’t be any shame around it. No one wants to have a mental illness and no one should blame themselves for having a mental illness.
I feel we need more research to be done in this area. Mental health and homelessness sometimes go hand-in-hand. There needs to be more state funding to help homeless families struggling with mental illness. Luckily, there are organizations like Sound Mental Health and NAMI fighting the good fight.
What You Can Do
- Join the Institute for Children Poverty and Homelessness on Thursday, June 8, 7:30-8:30 a.m. for a free webinar as they explore their recent data report “More than a Place to Sleep,” shedding light on homelessness and mental health for students. Register here.
- Read this Firesteel article about the long-term impact of Adverse Childhood Experiences, or ACEs, written by former project assistant Perry Firth.
- For more about child and youth homelessness and the health/mental health impacts, in America, read the America’s Youngest Outcasts report.
- Read this fact sheet on mental health and homelessness from the National Coalition for the Homeless. It includes an interesting section on how homelessness and mental illness can negatively affect an individual’s physical health as well.
- Learn more about Coordinated Entry for All in King County, which connects people who are homeless with housing and services such as mental health counseling.

Pingback: Published Written Pieces | Khadija Diallo